|
I just found this essay I wrote back in June of 2022. As you explore the inner world of yourself and others, you will see there is a sort of underlying 'first principles' or rules from which our organization emerges.
Give Them Some Oxygen 6/2/2022 Embracing the Hidden Wisdom Within: We all have parts that we don't like and try to smother. Parts that hold emotions that we reject, like anger, hate, weakness, sadness, shame, and wild pleasure. When we smother these parts, we dissect ourselves into arbitrary borders and dub some worthy and others unworthy. We become polarized and lose sight of what is wise about these othered parts. The Cost of Categorization: We do this because we feel those parts are costly. In our attempts to decrease our vulnerability, we become polarized in our thinking. We make some parts “good” and others “bad.” It is the categorization and labeling of these parts that is the origin of all functional mental illnesses. The parts that get smothered don't die, nor do they grow weaker, they instead struggle against their restraints and gag. They pop out sideways, acting out and demanding freedom to enact their wisdom. Reclaiming Wisdom: It's true that the unbridled expression of many of the parts that we reject, we learn to do because their expression was costly at some point. In our time of low understanding and lack of support, we make up stories about these parts so that they can never do the damage that they had done in the past. Ultimately, however, those urges that those parts have are wise in some way. They are pointing to something that we need either from others or from ourselves. As we mature and gain understanding and resources, someday, we can relieve the gag order and give these parts some oxygen. When we give these parts oxygen, it can be really scary. When those parts come, we feel the emotions that come with them. Perhaps there's hate, perhaps there is rage, perhaps there is a kind of blissful Mania that has no place in our home or business. When these parts come in, we feel those feelings we get scared that maybe we'll get stuck there, maybe the power I gained over this part will go away, and I will be overwhelmed by it. So, of course, in the beginning, it's important to do it with support, like Virgil holding Dante's hand in the Underworld. The Alchemy of Self-Discovery: We need someone who knows what they are witnessing to coach us through the intense sensation of the part as well as the intense reaction that we tend to have to that part. And with our hands held in this way, we are able to finally or at least start the process of seeing what this part is all about. And when we finally give this parts some oxygen, we begin to understand. Oh! We can hear the wisdom of what this part holds that we locked away when we locked away the dangerous aspects too. We get the opportunity to sort out that which is useful and that which is costly. In that sorting, this part has the opportunity to alchemize and transform into something updated that we can use now in our present lives. Trusting the Allies Within: We begin to see our parts as a gaggle of children in our charge. Never wanting to smother or deprive any of them but rather to lovingly understand and listen to the fate-altering, mind-blowing information that they have for us. And in so doing, finally, we get to reap the benefits of all parts of ourselves, updated and shown where we are now in our lives. We learned to trust these parts and give them access to the viewing room of our world. And when they see what we have become, they grow up to become whatever it is that we and they need them to be. We stop seeing these parts as enemies and instead see them as allies. We make amends for the misunderstanding and the defamation that we perpetrated on these sweet little beings.
0 Comments
 I originally got this metaphor from my mentor, Steve Finn. Thanks, Steve! Think of your emotional capacity like a bucket that can only hold so much. Everyone has different-sized buckets, and buckets can grow and shrink. When this emotional bucket overflows, it can lead to various reactions, from feeling depressed to getting anxious to getting angry. This post explores the importance of understanding these emotional limits, what happens if we ignore them, and the steps to help us recover. Inside the Emotional Capacity Bucket - Limits and Reactions: Everyone has a limit to how much stress they can handle and must find the right stress balance. Lack of “good” stress is also a form of “bad” stress, but that's for another article. Going beyond this limit can make some people feel sad, while others might get mad. In extreme cases, it might make someone think about making big changes in their life, like leaving their job, filing for divorce, or even suicide. Accumulating Stress: Once the emotional capacity bucket has been maxed out, every new stressor adds water to the emotional bucket, bringing you closer to “overflowing.” Even good stress pushes the person closer to the edge. People react differently to stress, so it's important to recognize that each person has their own limit. Expecting someone to behave or have the same capacity as you is misguided. Coping Requires Emotional Strength: Figuring out how to deal with problems requires emotional strength. If you’re already overwhelmed, it can be hard to express what you need or want. This is why typical “fix it” or “bootstrap (do-it-yourself)” interventions don’t work when someone is maxed out. Has anyone ever given you a lecture on mindfulness or told you to “take deep breaths” while you were overwhelmed? Or maybe they started giving you solutions saying, “Well, if you just did ‘xyz,’ you probably wouldn’t be feeling this way.” How did that feel? I personally believe coping should be used sparingly because it is much more efficient and effective to validate and allow difficult emotions to process through rather than trying to quell them with coping strategies. “Quelling” or soothing is really just gentle dismissing. Allowing emotions to process unburdens the person. The therapist or friend acts as a saucer who catches the overflow from the emotional capacity bucket. Listening and validating are the tools that help the excess water out of the bucket into the saucer of the person with more capacity in that moment. The beautiful thing about receiving the support of a good “saucer” is your bucket's capacity grows. Not only do you get relief in the moment, but you also are less likely to be overwhelmed by the same things in the future because you had the experience of surviving the hard situation and were supported enough to digest and reflect on what was hard about it. When you encounter something similar, your body and nervous system draw on the memory that you got through it before while in connection with a caring other. The embodied felt sense of that connection makes your emotional capacity bucket bigger, often even when no one is around. I want to note that in a world where good "saucers" and people with large buckets are limited, the vast majority are coping. I agree with Hafiz: “Fear is the cheapest room in the house. I would like to see you living In better conditions.” ― Hafiz Seeking Therapy Requires Emotional Strength: Telling an overwhelmed person to “just go to therapy” is harmful. Going to traditional psychotherapy requires some wiggle room in the stress bucket. If someone is already dealing with a lot, therapy might not be as helpful. It's a bit like trying to teach someone to swim when they've fallen off a boat—it might not be the right time. Getting bodywork that is focused on relaxation, neurofeedback, or supporting the person in carving out time for exercise, forest bathing, or alone time to do whatever they want can be much more helpful. Somatic Trauma and Attachment Therapists know how to work with the body without speaking and provide a viable alternative to traditional therapy for an overwhelmed person. See Emotional Injuries Like Physical Injuries When someone’s nervous system is maxed out and their bucket overflows, you must treat that person’s emotions like a broken bone or like the person who fell out of the boat in the earlier example. It is much harder for people to see emotional injury the way we see physical injury, but they are the same and often impact the nervous system similarly. Once you see it this way, you will feel silly if you find yourself arguing, dismissing, lecturing, or explaining to someone with an emotional injury. It will feel the same as arguing, dismissing, lecturing, or explaining to someone with a broken bone, like so: “Why are you crying? Everyone breaks bones. Don’t be such a drama queen.” “Why are you crying? Everyone gets anxious. Don’t be such a drama queen.” “Why can’t you help me with the groceries? It’s only a little broken.” “Why can’t you help me with the groceries? You’re just a little stressed right now.” “You know, I broke my arm once, and I was fine with it. It really made me a stronger person overall.” “You know, I had a panic attack once, and I was fine with it. It really made me a stronger person overall.” “Well, if you had paid more attention and not let things get out of hand, you wouldn’t have broken your bone. I’m not sure I want to take you to the ER. You need to learn your lesson.” “Well, if you had paid more attention and not let things get out of hand, you wouldn’t have become suicidal. I’m not sure I want to take you to the ER. You need to learn your lesson.” “Aw, come on, don’t complain about your broken bone. How do you think I feel?” “Aw, come on, don’t be angry. How do you think I feel?” “Oh wow! Your broken bone hurts so bad you've been in bed for days. Have you tried breathwork?” “Oh wow! You’re so depressed you've been in bed for days. Have you tried breathwork?” “You still have chronic pain? You’ve had that for 18 years! You should just get over it.” “You’re still sad about your childhood? You’ve been an adult for 18 years! You should get over it.” If you're the person with more emotional capacity, you may be thinking, “Well, it's not MY responsibility to coddle the emotionally injured person! What if I give in to their theatrics and make them weaker?” That is exactly the point I am making here. Validating and helping the person process the emotion makes them stronger. Dismissing and denying makes them weaker. You are actually making more of a problem for you and them down the road by trying to get rid of their problem rather than treating it like the injury that it is. It is the same as ignoring a broken bone. If I ignore a broken bone, it heals in such a way that the bone is weaker and more likely to break again. If I try to use the limb with the broken bone before it is healed enough, I reinjure the bone, and the recovery time is longer. Recognizing the Need to Stop: When something is wrong with our mental health, the first step is to recognize it and take a break to figure things out. Just stop. Then observe. That pause is so important. It can feel like swirly chaos, nauseating, clenched, imploding, exploding all at the same time. This is why people avoid stopping, but it is 100% necessary. Then observe. Take on a beginner's mind. Watch how you think, feel, and behave without trying to make any changes at all—just notice. Take the Pressure Off: Just like we wouldn't put weight on a broken leg, we should avoid things that add stress to our minds during the recovery time. Clear your schedule if possible. Taking medication might be a good idea. If you have to work, do the bare minimum. Take as many goals and deadlines off your plate as you can. Focus on the present moment for the most part. You may need to update your identity. The sooner you can take the pressure off, the sooner you will be able to reengage with life. The clients I have worked with who can stop quickly (and quickly is usually a six-month process!) have less to recover from because the pressure has not been piled on top of being totally maxed out for years or even decades. Clients who have been maxed out and who have had to “carry on” in that state with added pressure to “keep it together” take a lot longer to heal. I often have to sell stopping to people because social pressures to perform, achieve, and produce make people who stop feel shame. Choose the Right Professionals: Seeking help from professionals, like talking to a doctor for a broken bone, means working together to figure out what will help. It is important to find someone who understands the power of listening and validating. It does not matter how many degrees, how much clout, how many fancy techniques or medicines they wield. If your provider does not listen to you, they will waste your time and cause a lot more damage. If you feel ignored, dominated, or dismissed by your provider, leave immediately. This can be so, so, so hard when you’re already emotionally maxed out. You may not be able to do it, and that’s ok. Once you can muster the strength, start interviewing other providers. How you feel with a practitioner matters. Taking Small Steps to Recover: After taking a break, it's important to take small steps toward feeling better. This is like doing exercises to help a broken bone heal. You should move to this phase only once the bone is strong enough to do gentle physical therapy. On the other hand, not moving to this phase when it is time is also injurious. There are a lot of reasons people might avoid moving on to the active recovery phase:
Make Intentional Life Changes to Stay Healthy: Once the gentle recovery process has begun and we start to feel better, we can start to think about overall changes to make in our lives. Intentional changes that begin to emerge as a part of the healing process come with the belief: “Something wasn’t working, and I have agency to live a life that works for me.” Intentional change takes into account ongoing stressors like chronic illness, demands of your culture, needing to work, paying down debt, and other facts of life that might be present for you. Intentional change does not come from a place of ignorance or naivety. Rather, it takes stock and inventory of what is true now and what is possible from here. This differs from the changes made during a crisis. Changes made during a crisis often involve projecting all of the “bad” and blaming one person or situation or making broad sweeping generalizations about all of life itself (which can lead to suicide). Changes made during a crisis come with a belief that “if I just get rid of this one thing, it will ‘throw-away’ all the bad stuff in my life.” Understanding and respecting our emotional capacity is not only a personal responsibility but also a collective endeavor to develop a culture that truly understands and prioritizes mental well-being. Through awareness, validation, and intentional actions, individuals can navigate the complexities of their emotional worlds, promoting resilience and creating a foundation for lasting positive change. "The only way to make sense out of change is to plunge into it, move with it, and join the dance." - Alan Watts
Why do I keep getting into abusive relationships? Why do I stay in a job that I hate? Why do I keep choosing addiction when I know that I really want connection? I need to change, but I am scared and frozen. Why is that? Ancient Fear Human fear of change is a complex and multifaceted phenomenon rooted in evolutionary, psychological, and sociocultural factors. Avoiding change helped our early ancestors survive. They were much more subject to rapidly and dangerously changing conditions and needed to seek security to survive. Our ancestral instincts are incompatible with the conditions under which we now live. The result is that modern people stay “frozen” unnecessarily, or even to our detriment, in habit loops, unable to move on to a more enjoyable existence. The following reasons for fear of change come from our harsh beginnings and the nature of human social relationships that developed to meet our original challenges:
It's important to note that the degree to which someone fears change can vary widely, and some people are more adaptable and open to change than others. Furthermore, the context and nature of the change play significant roles in shaping individual reactions. Regardless of your circumstances, embracing change is a practice that improves when we bring intentionality to it. How do I increase my capacity to change? “Fear is a mile wide, and an inch deep. We perceive it as a massive ocean. Then we step into it, we realize it's just a puddle.” - Leila Hormozi Increasing one's capacity for change involves a combination of self-awareness, intentional effort, and a willingness to embrace new experiences. In many ways, embracing change is going against human instinct. You are not less of a person for feeling insecure while going through change. Rather, insecurity is to be expected because resistance to change is hardwired into us as a species. Here are some strategies to enhance your ability to navigate and embrace change while managing the inherent vulnerability and insecurity of the change process: Process Freeze States:
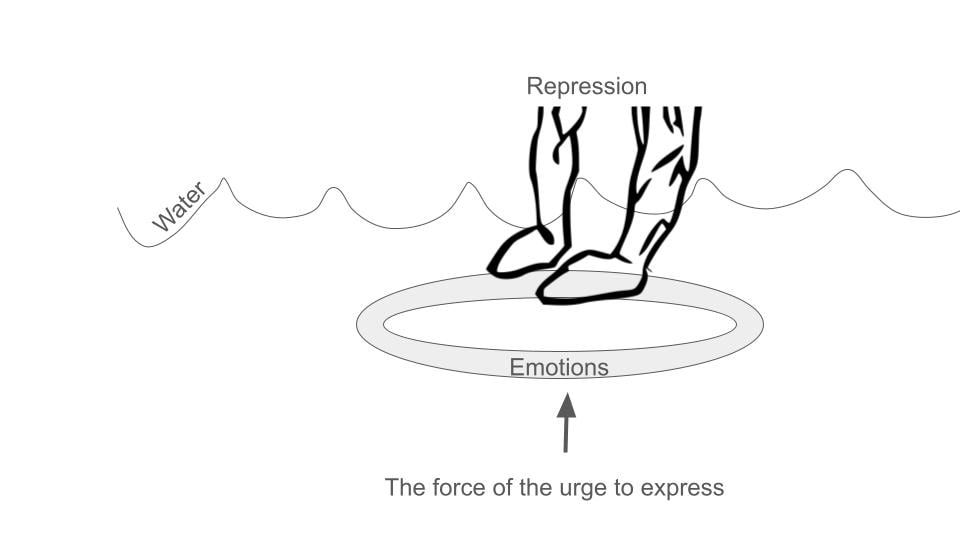
Change is a gradual process, and it's okay to take it one step at a time. Consistent effort, self-compassion, and a willingness to learn can significantly increase your capacity for change. Sometimes, a sense of urgency and the desire to rush change is a way to avoid change. This can stem from a fear of the change process. The urgency is trying to skip over the painful parts of change outlined in the first list above. Change can feel like jumping off cliffs. You can develop your relationship with the change process by jumping off curbs instead of cliffs to start to get used to the feeling of “falling.” Facing your fears does not mean you must be frozen in terror or bowled over by overwhelming emotions. If you look at change with an experimental attitude, you can take the pressure off of being perfect. Experimentation invites and expects mistakes. It values mistakes and failures as the fastest way to arrive at modes of living and functioning that work best for the given moment in time. Expect Complex Emotions and Be Ready by Knowing Your Own Complexity Have you ever heard clients (or loved ones, if you’re not a therapist and want to participate in the exercise) say things like this? What are the underlying emotional states you see in each example? (Suggested answers are at the bottom of the article.) 1. “I just feel so much rage, I literally see red. Like my vision is covered in a red film.” She said, visibly shaking in her seat. “If my colleagues knew, I don’t know, I could lose my job, or worse, my reputation. I’ve done things I’m not proud of.” 2. “I’m bad…” he stares off into space, “evil. There’s evil in me. I feel like I deserve all the bad things that happened to me. It's hopeless; I’ll never get better.” he pauses again, “I dont know if I want to get better. I want to die and take the whole world with me. Burn it all to the ground, you know?” 3. “When I think about what happened,” they said grimacing, “I dunno,.. Ugh!” they stuck their tongue out as if to vomit and lifted their hands, repulsed “It's just so disgusting, it's unbelievable! I CANNOT believe it.” 4. “I think I hate him…I HATE HIM!” he exclaimed, suddenly stopping in his tracks like a record scratch. His eyes stared off to a corner in the room, and all the life drained from his face. His voice faintly floated out of his throat, saying, “Oh wow, I was so worked up, but now I have no idea what we were talking about.” In the world of therapy, emotions are complex and varied, often bringing forth a rollercoaster of feelings for clients. As a therapist, it's crucial to expect and embrace the full spectrum of emotions that clients may experience during sessions. Here, I will explore the importance of acknowledging and creating space for feelings such as shame, anger, sadness, vulnerability, confusion, disgust, and even suicidal ideation. We'll discuss why attempting to "fix," "soothe," or "dismiss" these emotions is counterproductive and explore the role of dissociation in emotional processing. Moreover, we'll discuss practical strategies for therapists to navigate intense feelings, incorporating somatics and parts work into the therapeutic process. Embracing a Range of Emotions: Clients seeking therapy may experience a wide array of emotions that are often considered uncomfortable or challenging. It's essential for therapists to anticipate and acknowledge feelings of shame, anger, sadness, vulnerability, confusion, disgust, and even thoughts of suicide. By expecting these emotions, therapists can create a safe and non-judgmental space for clients to explore and express themselves. As you practice, you will start to recognize the “aesthetic” of an emotional state. The aesthetic is a multifaceted experience of the person that includes thoughts, emotions, sensations, postures, movements, body tension and collapse patterns, images in the client's and therapist's minds, and more. Sometimes people refer to the aesthetic as the "energy" or "vibe." The ability to recognize the aesthetic enables you to determine what emotional state is present faster and to validate the client experience more fully. For example, I can reflect that a client is sad because they are tearful. If I have a more complex relationship with aesthetic and I am attuned to the overall aesthetic of "sadness" in this person, I can reflect a shift to sadness before the client is fully in it, which increases rapport and trust in that the client feels acutely tracked and also feels “felt.” Furthermore, not all clients cry when sad. Acknowledging sadness when the client's expression might be more subtle, or the person’s sadness is generally not recognized or honored, can increase the client's awareness of sadness and help the client feel safe to feel the sadness now and increasingly as time goes on. This goes for any emotion, especially socially “inappropriate” ones. Thus, we heal the consequences of death by a thousand paper cuts that shove emotions down underwater. Many people have not been explicitly told to “not feel that feeling” but have gleaned from their environment that it is not okay to feel certain feelings. This is primarily done through dismissing, fixing, and soothing. The result is like trying to hold a life raft underwater: Avoiding the Urge to Fix or Dismiss: The impulsive reaction for many therapists, like those who trained the client not to feel in the first place, might be to alleviate their clients' discomfort by attempting to fix, soothe, or distract them from their emotions. However, these well-intentioned efforts can hinder the therapeutic process. Therapists should resist the urge to "fix" and focus on naming, validating, and feeling along with the emotions the client is experiencing. The exception to this rule is when a client dissociates; I will address that later. The reason that I see therapists have a hard time with this is that therapists have discomfort with their own socially unacceptable emotions. The only way for a therapist to get really good at validation is to be willing to feel fear, shame, disgust, and even suicidal ideation. The therapist needs to be unafraid to feel these feelings. Are you afraid to feel fear, sadness, loneliness, hopelessness, and the inner condition that causes suicidal ideation? If so, that means you don’t trust yourself to go into the emotional state and then come out of it. Another way to say this is that you don’t know how to regulate your nervous system at that level. Nervous system or emotional regulation does not mean that you are always serene and placid. It means that you can go into ANY feeling and efficiently find your way out. Ideally, what happens is the therapist feels a little bit of their version of the client's feeling, like rage, for example. Here’s how it goes down: The client looks tight; their jaw is clenched, biceps flexed, shoulder rounded forward, fists are starting to ball up, and their brow is furrowed as they talk about how, once again, their partner is making unreasonable, selfish demands. You say, “Wow! A lot of rage, huh?” Client: “Oh…my…god, I could punch a wall right now.” Therapist: “Oh yeah! Anyone would feel that way. I’m angry too hearing about this. Is it okay with you to feel this anger right now?” Client: “Yes, but I feel so stupid getting charged up like this.” Therapist: “Sure, that makes sense, you were taught it's not ok to be angry.” Client: “Right, anger was off limits. Mine was, anyway. What's the point of this anger anyway? It doesn't fix anything.” Therapist: “It's really uncomfortable to feel that much anger, huh?” Client: “Yeah, what do I do now?” Therapist:” What does your anger want you to know?” Client: “I am lonely and hurting.” Therapist: Oh yeah, can we just feel that loneliness and hurt together? Client: “Yes, that’s ok.” Therapist: “What’s it like to have someone feel this loneliness with you?” Client: “It's nice.” Therapist: “What's nice about it?” Client: “I do not feel alone; my anger can calm down. I feel like I can see my relationship in a different way.” This is an abbreviated example of validating, joining, and connecting the dots for the client and inviting the message of the feeling. There are many ways that this example does not capture how complex a dialogue like this can be, but the overall flow and format I present is something I experience repeatedly in sessions. Feelings are messengers. If we told the client to “try some deep breaths” when they wanted to punch the wall, we might not have arrived at the vulnerable feelings underneath. and we would not have been able to help the client feel connected. Notice how when the client feels connected and regulated, they can reframe their situation on their own. The therapist did not have to give them advice. This is the power of good implicit and explicit reflection statements, validation, and feeling with the client. It winds up being a lot less work for the therapist. Many therapists burn out, even in private practice, because they think they need to know everything or at least know a lot. Interpretive knowledge can help you steer the ship, but in actuality, you just need to know how to follow the client. That kind of knowledge is much less “expensive” than having to figure out how to interpret everything all the time. Understanding Dissociation: Many clients have learned that their feelings are not acceptable or valid, leading to dissociation as a coping mechanism. Therapists need to be vigilant for signs of dissociation, as it can be damaging if left unaddressed. Monitoring for dissociation and understanding its nuances is crucial for effective therapy. Rather than reacting to dissociation with panic or discomfort, therapists should strive to become competent and confident in handling it. Signs of possible dissociation include client reports and visible clues. Clients might report feeling confused, foggy, or suddenly feeling blocked while processing. Clients might not have words for what they are feeling, but you will get the hint they are dissociating because they suddenly look scared, frozen, or far away. Their speech may become slower, and more disorganized, their sentences might seem incomplete, or they may change subjects rapidly, becoming difficult to understand. It is important to know how to name the dissociation respectfully and artfully bring it to the client's attention. When a client dissociates, it means that something just “happened,” usually something that is “intolerable” for their system. Reassure the client that they always have consent and dont have to feel something they don’t want or aren't ready to feel. This reassurance can take the pressure off of the dissociation. I usually ask the client, “What was intolerable about what we were talking about just now?” Usually, the answer has something to do with “I’m not supposed to feel ______,” “I’ve trained myself not to feel_________,” “It’s too vulnerable to feel________,” etc. Rarely does a client recall a memory of which they weren't aware. Rather, it's usually an emotion or sensation that the client trained themselves not to feel long ago. Titrating Intensity with Somatics and Parts Work: To ensure the emotional intensity remains tolerable for clients, therapists can integrate somatic techniques and parts work into their practice. Somatics involves paying attention to the body's physical sensations, helping clients ground themselves in the present moment. Parts' work explores the various aspects of a client's personality or identity, facilitating a deeper understanding of their emotions without being consumed by them. The work, then, is to help the client learn to tolerate what has previously been intolerable. My aim with clients (and myself) is to be able to be present with any emotion or sensation. Once someone no longer has “off-limit” feelings, they experience much greater ease, clarity, and flexibility in life. It’s much easier to be continuously present. They can feel a feeling and efficiently find their way back to a healthy baseline, which is much easier to achieve if the therapist is constantly modeling regulation this way. It's a simple goal arrived at by a varied and nuanced path for every individual: Therapists play a vital role in helping clients navigate complex and challenging emotions. By expecting and embracing feelings of shame, anger, sadness, vulnerability, confusion, disgust, and suicidal ideation, therapists can create a supportive environment for clients to explore and express themselves. Avoiding the temptation to fix or dismiss these emotions, monitoring for dissociation, and incorporating somatics and parts work are essential strategies for therapists to foster a more profound and effective therapeutic journey for their clients.
Liz's Parts Work Journey
Studying non-dualistic spirituality in the tradition of Ramana Maharshi and my experience with clients during the first years in bodywork practice inspired me to see humans as multiple. Seeing humans as multiple contextualized a series of consciousness events I had growing up and in my early adult years. I am sharing this story because it highlights an underlying organization I feel in life. I believe that when someone discovers and interacts with this harmonious organization (aka spirituality, the "universe," the Game, the Tao, God, divine order and timing, etc.) in whatever way they name it, that the process of interacting with "it" is healing in and of itself. I discovered somatic parts work through a suggestion and a surprise. One day in 2010, my mentor, Steve Finn, told me, “Parts don’t go away, but we can throw them a retirement party or help them change their job description.” I adopted a “no parts left behind” policy from that day forward. At that time, I was also hyper-focused on non-dualistic spirituality from Ramana Maharshi's lineage and Eckhart Tolle's teachings. To see the good and the potential in others is a core tendency of mine, and this focus deepened my tendency to “see” the core essence of light and being in others. I have also been generally aware of the layers of disruption, anger, pain, and separation that layered on top of the core. The awareness of the layers increased at this time, too. I remember being confused as a young person because you couldn’t just interact with anyone and have an easy connection. I always felt like easy connection ‘should’ have been the case because I could “see” the core of perfection in others. Learning how the other “layers” or parts functioned helped me understand why the connection was so hard. Shift to Direct Communication with Parts As my clientele shifted to people with more significant trauma presentations, I began talking directly to parts. I would ask the parts and the client permission and invite the parts to speak freely. This was particularly easy with clients who had structural dissociation (the extreme version of this is called DID - dissociative identity disorder). It seemed to me that the parts needed someone willing to listen and go to the dark places with them. I was surprised that they tended to resolve on their own with good presence. I noticed that parts have their own postures and movement patterns, their own fascial restrictions, they hold disparate belief systems, and sometimes they even have their own mind/body dis-ease processes separate from other parts. Incorporation of Sensorimotor Psychotherapy (SP) My education in Sensorimotor Psychotherapy changed how I do parts work and added a new level of sophistication. I named my new Colorado-based therapy practice PROSOPON because I wanted to juxtapose the “prosopon” (πρόσωπον) or “parts that change,” i.e. masks or faces from the hypostasis (ὑπόστασις), “the essence that stays the same,” i.e. the non-dual core. This is one of the interpretations of this philosophical concept. (I also like how the “Os” in PROSOPON look like faces…to me anyway.) Philosophical Underpinnings and Education By the way, you see a lot of Greek and philosophy in my writing because I studied Latin for four years as a teenager and ancient Greek at my college, which is primarily a philosophy school (also called a great books program). I had the opportunity to study at the Zen Center in town concurrently. I am a great lover of evolving wisdom traditions and I bring them into my practice. Introduction to Internal Family Systems (IFS) I laughed out loud when I realized "how much time I wasted" (it's not really wasted time. The work was worth it and I wouldn't take it back for anything). I finally attended a 14-hour introductory course in Internal Family Systems this summer, the most recognizable version of parts work. I spent over 12 years developing my own approach when I could have just taken an IFS training. Fortunately, life is about the journey, not the destination. I took an introductory Janina Fischer training about her combination of IFS and SP (called TIST or Trauma-Informed Stabilization Treatment) this spring too. I must not have been ready to “get it.” I loved the training and incorporated what I learned, but it did not land like IFS. Accelerated Healing with Combined Approaches Incorporating the ideas of IFS, TIST, Sensorimotor, and my own style of approaching parts has accelerated the healing and recovery I have witnessed in my office. I am so excited to feel validated and educated by Dick Schwartz, his approach, and his community of therapists and trainers. The Implicit "Rulebook" for Parts Work The interesting thing for me is this: if I can develop my own version of parts work by interacting with client parts, as many therapists do, there must be an underlying implicit “rulebook” for how the human multiplicity of subpersonalities function. This reflects my experience with spirituality as well. When you simply turn your attention to something like the Tao, let’s say, over time, you start to get an embodied understanding of it that no word-based explanation can provide. The fundamental rule is that we are all multiple, and many of our mind-body and behavioral difficulties can be resolved if we start honoring, loving, and updating our subpersonalities as though they are real people. Key Modalities: IFS, Sensorimotor, and TIST I want to be really clear and transparent that I have yet to take level one of either IFS or TIST as of December 2023. I have taken introductory courses and studied material related to IFS and TIST, but I do not claim to practice these modalities per se. I incorporate my understanding of the philosophical and practical underpinnings of each modality. I love the IFS unburdening process because it's straightforward and user-friendly. Sensorimotor is magic surgery. SP properly applied manages a nervous system and its transformation better than any other modality I have ever witnessed. IFS helps SP get the job done by helping a client get to know their system, how to ask parts for genuine consent and learn about your non-dual core and how your parts relate to that core. The IFS framework creates an environment within which SP can do its magic. Importance of Regulation and "Titration" TIST highlights the importance of using parts for regulation and “titration” largely because Janina Fischer’s clientele, like mine, often have strong dissociation and overwhelm components. When an overwhelming feeling is present, we can't process it all at once. It's like being presented with a gigantic sandwich. I couldn’t eat the whole thing in one bite, but I can finish the sandwich if the bites are smaller and spread it out over multiple meals. When I recognize that an overwhelming feeling resides in just one part of me instead of all of me, it's like eating one bite of the sandwich rather than trying to choke the whole thing down. Pure Bottom-Up Somatic Work in Certain Cases There certainly are exceptions to this IFS and SP ordering. From time to time a client comes in, and they are so good at avoiding, or their nervous system is so disorganized that using emotional or sensing talk of any kind is unavailable. In these cases, I start with pure bottom-up somatic work, either myofascial release or somatic movement of some kind. Myofascial release is especially suited to help these clients because hardly any talking is required, and any talking that we do is related to purely physical things. Every time I have used this approach, the client begins to bring up emotional things on their own in their own time. You can read my article on trauma and fascia to understand more why starting with a pure MFR approach can be helpful for these presentations. I embrace the haphazard and, at times, comical nature of my journey (read “ignorance”), cherishing the continuous evolution of my 'selves' and therapeutic approach. The invitation to clients and clinicians is this: honor the journey, recognize the multiplicity within, and leverage the transformative power of somatic parts work. Trauma affects your fascia, but why should you care?
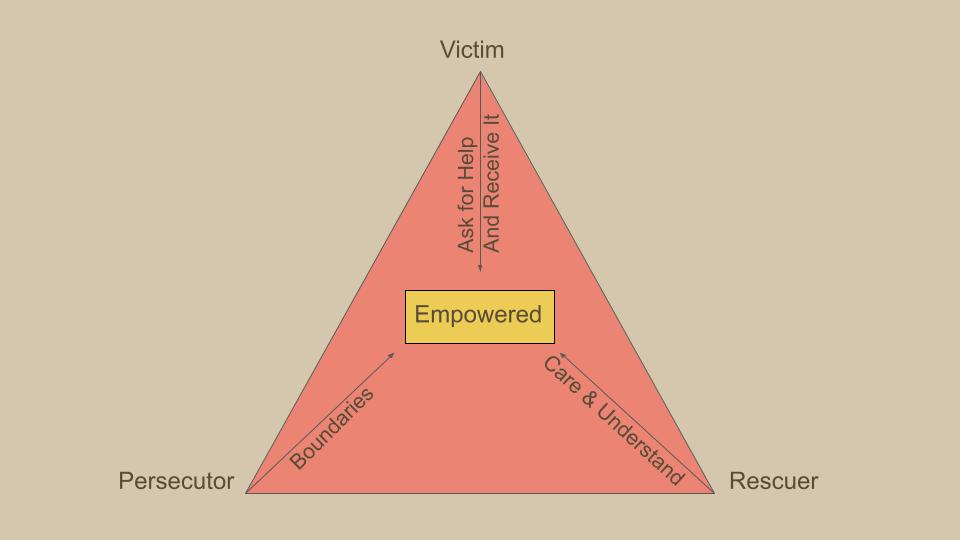
I care personally because addressing my fascia was key to my trauma-healing needs. I continue to regulate my nervous system with fascia care. I have seen the way my clients benefit. For some of my most complex cases, a course of hands-on fascia work allowed us to begin a healing process that sometimes ended decades-old symptoms. Clients have told me that the work can feel “psychedelic,” providing sudden insight, and “more relaxing than Xanax.” Those were just a couple of comments in the last few weeks. I could do a whole post on clients' reactions to the work (and I shall!). That seemingly simple body and touch work can produce effects as powerful as drugs without the hangover (usually) has completely altered my reality since I learned it in my mid-20s. It feels ordinary to me now, but I am constantly reminded of how amazing it is because my clients continue to react so strongly to it. “But why is fascia work so powerful?” you might ask. When I first encountered the power of fascia work, I asked this question, which kicked off a decade of voracious study on the topic. I will now attempt to give you a few distilled key points that can answer this question. The fascia and the nervous system occupy the same space in the body and are extremely intertwined. The fascia, a connective tissue, is intertwined with the nervous system as it contains sensory receptors called proprioceptors. These receptors provide information about body position and movement to the brain, contributing to the body's overall sense of spatial awareness. Additionally, fascia has been suggested to influence neural signaling and may play a role in conditions involving chronic pain or body system dysfunction (circulatory, digestive, lymphatic, immune, endocrine, etc.). Therefore, psychological trauma shows up in the fascial system. Psychological trauma can manifest in the fascial system through various mechanisms. Trauma may lead to increased muscle tension, affecting the fascia and potentially causing it to become tight or restricted. Chronic stress from trauma can contribute to the development of myofascial trigger points, which are hypersensitive areas in the muscles and fascia. Moreover, the body's response to trauma, particularly the fight-or-flight response, can create patterns of muscular tension and altered movement, impacting the fascial system. Emotional stress and trauma might also influence the autonomic nervous system, which can affect the fascia's tone and function. Research on the connection between psychological trauma and the fascial system is ongoing, and it's an evolving area of study within fields like psychoneuroimmunology and somatic psychology. Many of us in the Fascia and Somatic Fields regularly witness spontaneous memory recall when areas of an individual fascial system are released or when positions of past trauma (or even positions of neutral or pleasurable events) are experienced in a person's posture or body positioning. Fascial touch and movement techniques act on the Ruffini Endings and why that matters. Fascial release techniques, including stretching, “unwinding,” and a specific type of massage, may influence the fascia through various mechanisms, including stimulating Ruffini nerve endings. Ruffini endings are a type of proprioceptor found in the fascia that responds to sustained pressure and stretching. When myofascial release is applied, it can lead to a decrease in tissue tension and increased flexibility. The pressure and stretching stimulate Ruffini nerve endings, sending signals to the central nervous system that contribute to a relaxation response. This can result in a reduction of muscle tension and improved mobility in the fascial system. Since the fascial system is involved in all systems, including the nervous system, which is where psychological trauma is “stored,” trauma affects your fascia. Based on my personal, my colleagues, and my clients’ experiences, the current theory is that releasing fascia allows us to release some aspect of trauma stored in the central nervous system. Fascia also affects your trauma. The fascial system can put up to 2000 lbs per square inch on the body by means of restrictions that form in response to injuries and chronic psychological patterning. The brain registers this crushing force as danger and stress. When the circulatory, musculoskeletal, and other body systems no longer suffer the crushing pressure of fascial restrictions, they stop alerting the brain that they are in danger, thereby decreasing the overall stress load in the body. Big Caveat: much like mold illness, autoimmune disorders, and other stress disorders, while it is wise to treat restrictions at the body level (like treating mold symptoms through detoxification protocols), regulating your nervous system is ultimately more important. If you treat your restrictions without knowing how to regulate your nervous system, you'll be treating restrictions forever and wondering where is the benefit. Ideally, both happen at the same time. Why You Might Care. The profound interconnection between the fascial and nervous systems highlights the significance of addressing trauma through fascia care. The revelations stemming from personal experiences, as well as the transformative impact observed in clients, emphasize the potency of fascial work in trauma healing. The manifestation of psychological trauma within the fascial system, whether through increased muscle tension, the development of trigger points and chronic unexplained pain (think fibromyalgia and myofascial pain syndrome), or altered movement and posture patterns, emphasizes the intricate relationship between mind and body. The ongoing research in fields like psychoneuroimmunology and somatic psychology further validates the evolving understanding of how trauma “resides” within the fascia, so to speak. The tangible results witnessed by those in the Fascia and Somatic Fields, including spontaneous memory recall during fascial release, inspire hope in the potential of these techniques in unlocking and processing deeply embedded traumas. Fascial touch and movement techniques, by acting on the Ruffini nerve endings, offer a unique avenue for trauma release. The stimulation of these proprioceptors through pressure and stretching initiates a cascade of responses in the central nervous system, ultimately leading to a relaxation response. This process reduces tissue tension and enhances flexibility and mobility in the fascial system, which is intricately linked to all bodily systems. Thus, all body systems potentially experience renewed freedom in their function. In the process of trauma healing, the revelation that releasing fascia may facilitate the release of stored trauma in the central nervous system presents a compelling perspective. The comparison of fascial work to the powerful effects of drugs, without the undesirable side effects, speaks to the potential of this approach in promoting holistic well-being. As we continue to unravel the mysteries of the mind-body connection, the role of fascia in trauma becomes increasingly evident, providing new avenues for healing and resilience. Karpman's Drama Triangle is a psychological model that explores the dynamics of interpersonal relationships and the roles people often unconsciously assume in conflict situations. Developed by Dr. Stephen Karpman, this model outlines three primary roles within the drama triangle: the Victim, the Persecutor, and the Rescuer.
This is a framework that clients often find helpful. Victim: The Victim in the drama triangle feels powerless, oppressed, or mistreated. They often portray themselves as helpless and may seek sympathy or external validation. Victims tend to avoid taking responsibility for their own circumstances and may inadvertently contribute to their feelings of powerlessness. Victims avoid personal growth by clinging to their victim status and blaming others.
Persecutor The Persecutor is the one who, consciously or unconsciously, takes on the role of the aggressor or antagonist. They criticize, blame, or attack others, creating an environment of conflict. Persecutors may feel justified in their actions and may not recognize the impact of their behavior on others. Persecutors avoid personal growth by devaluing and blaming others.
Rescuer The Rescuer is the individual who intervenes in the conflict, often with the intention of helping or saving the Victim. However, the Rescuer's actions can sometimes enable the Victim's sense of helplessness and may contribute to a cycle of dependency. Rescuers may also become frustrated if their efforts are not appreciated or if the Victim does not take steps towards self-empowerment. The Rescuer needs the Persecutor to persecute so that the rescuer can compare themselves to the persecutor and feel like a superior person. The Rescuer avoids personal growth by getting caught up in other people’s lives.
The Drama Triangle is dynamic, with individuals often moving between these roles in response to changing circumstances or triggers. What makes this model particularly insightful is its recognition that each role in the triangle can be disempowering and contribute to the perpetuation of interpersonal conflicts. Breaking free from the Drama Triangle involves individuals taking responsibility for their own roles and working towards more assertive, collaborative, and empowering communication styles. Doing so encourages self-awareness, accountability, and the development of more functional communication patterns. I am a fast processor, and I often attract fast-processing clients. People like us produce ideas rapidly. I also identify as a somatic person. I've spent a lot of time around people and groups that are intellectual and others that are somatic. Going through life as this combination creates dissonance. In somatic circles, I can be interpreted as disembodied. In intellectual circles, I can be interpreted as “out there.”
Internally, I feel congruent. When I observe misinterpretation, I notice it, feel a little disappointed, and reflect on how I truly feel inside. There is a temptation to get defensive. I want to explain myself. There is a misconception that you can’t be intellectual or a fast processor and simultaneously embodied. The truth is, you can presently embody whatever you are. You can even presently embody disembodiment. Speed has just as much a place in the body as slowness. Some bodyminds love speed. These body-minds often don’t do well with seated meditation and require other types of contemplative practice vessels. When you are choosing a contemplative style, choose one that feels good to you. White-knuckling through a 40-minute seated Zazen practice is not virtuous and misses the point unless your aim is to be present with limbic friction, which is also fine. Just be intentional that this is your aim. The point of a contemplative practice is to become present by repeatedly returning to a single focus. That could be a mantra or working on a Rubik's Cube. Your contemplative practice does not always need to be done as “time set aside” like a timed meditation. You could decide to return to your breath, sensations in your body, or something else, over and over while cooking or hiking in the woods. Doing focused timed practices is very helpful for learning presence and maintaining a strong connection to presence. If doing a timed practice is very irritating or brings up trauma, and that is not your aim, it's not time to have this as a part of your life. You may need some help from a therapist or spiritual person to work through your tangles inside. Once you have more inner clarity, you will love your practice in whatever form you connect with. Try a different practice if it feels like a chore or a battle. It might not be you. The practice vessel may be a bad fit. Types of Contemplative Practice Vessels:
What makes any of these practices contemplative is the quality of attention you bring to it. At first and in general, you practice keeping your attention on the thing you are doing. When your mind wanders, you bring it back. Over time, your relationship to contemplative practice evolves. You may feel an affinity for one specific practice vessel. Your preference may change to different practice vessels over time. It's important to know that it is not about any specific practice vessel (including seated meditation). The practice through any vessel is presence in the here and now. That is all. There is no aim other than this. The aim is not to “slow down,” “wake up,” “be better.” The aim is to be present and nothing more. “How can that be helpful?” You might ask. “Why would I want even to try this if it's not going to ‘help’ me?” Well, try it and see what happens. Let go of the mindful marketing out there that it's for this or that purpose, that you could become enlightened, or that you’ll be a better person. People have, understandably, used many tactics to convince others to do contemplative practices. They have used motivational and marketing hooks to get the job done. You may be reading this article because you want to be further convinced to practice. But why? Underneath all the teachings and mindfulness click-bait, there is something else entirely. I will not try to capture the “thing” or “not thing” in words. I can’t, and no one can. Lao Tzu famously points out the issue: The Tao that can be told is not the eternal Tao. The name that can be named is not the eternal name. The nameless is the beginning of heaven and earth. The named is the mother of ten thousand things. Try your hand at presence. Every time you do, invite total openness to what is. That is sensation, environment, inner experience, your life circumstances, the state of the world, that which you “know” and everything “you don't know,” and just see what happens next. If you're a fast processor or some other misunderstood type of person, don't try to “fix” yourself. There is nothing to fix. Be with who you are now and watch yourself become. Bodytherapy is Psychotherapy, and Psychotherapy is Bodytherapy.
There, I said it. This reality is a huge taboo, and its taboo status has been gnawing at me. Like many therapy professionals, my work is deeply connected to my personal journey. My life began with a foundation of confusion and fear, driving me to seek answers early on. At seven, I was fascinated by Maslow's hierarchy of needs, and by nine, I boldly declared that the cycle of my family's ancestral trauma would end with me. Despite having many friends and achievements, I always felt like an outsider, navigating life on shaky ground and unable to follow the "normal" path. My first encounters with therapy came during my teenage years, and I saw several psychotherapists in college. However, my condition continued to decline until I met a psychologist and an osteopath who treated me like a person. This, I believe, is the essence of good psychotherapy: seeing the client as a whole person. You might wonder, "If your other therapists weren't treating you like a person, what were they treating you like?" At times, I felt like I was merely a paycheck, a diagnosis, a problem, a juvenile delinquent, an ego booster, or a naïve teenager. I kept waiting for someone to ask, "And how does that feel in your body?" because I was experiencing so much physically, and I was surprised no one did. Working with those two professionals evolved into a mentorship that shaped my approach today. One helped me understand transference, countertransference, and parts work, while the other introduced me to Osteopathic Manipulation and Katsugen Undo. Both taught me mindfulness and spirituality, leading me to leave the traditional career path and start a massage and yoga practice. With their guidance, I moved away from medication, worked with a Functional Medicine doctor, and eventually stopped using FM protocols as well. By then, I had completed yoga teacher training, learned Myofascial Release, practiced energy work, and participated in extensive group therapy. I found freedom in using food, connection, and movement as my medicine, and for the first time in my life, I seldom felt fatigued because I was living in alignment with my values and regulating my nervous system. My clientele began to evolve, attracting people who had experienced trauma and were dealing with its psychological and physical consequences. During bodywork sessions, clients would sometimes shift into sub-personalities, discharge their nervous systems, or recall memories spontaneously. When someone becomes a scared two-year-old on your table, you help them. You don't tell them to "cut that out" because this isn't psychotherapy. I did my best but knew I needed more training. I attended the Interpersonal Neurobiology Conference and discovered Sensorimotor Psychotherapy. Shortly after, I woke up one morning and wept, realizing what I had to do. I shut down my thriving practice in Austin and moved to Boulder to study somatics. While in graduate school, I restarted my practice, earned my degree, and got certified in Sensorimotor Psychotherapy. I had the serendipitous opportunity to work with a Functional Neurological Disorders expert, which brought all of my education together, enhancing my ability to help others on their healing journeys. Learning to treat Functional Neurological Disorder (FND) was a pivotal moment for me, although I didn't realize it at the time. I hesitated to acknowledge it due to an unspoken taboo. Here's how this issue manifests:
I respect the needs of large mental health institutions and workplaces that train new clinicians. While graduate programs do have rigorous evaluation practices, they often fall short in screening out clinicians who misuse touch or power. Understanding why touch is particularly taboo in these programs would require further research. Do we doubt new clinicians' ability to discern which clients would benefit from touch? Or are educators reluctant to learn about the appropriate use of touch themselves? In residential programs, the taboo around touch is more understandable. During my time at inpatient treatment centers for people living with psychosis, it was evident that residents needed nurturing touch. However, allowing touch between patients posed risks, such as it turning into sexual contact or inappropriate boundary testing, which I witnessed frequently. While I believe we should strive to permit platonic touch despite these risks, I also understand why overworked and understaffed clinicians might avoid it. At a high-end facility for individuals with psychotic disorders, clients could leave the campus for massage therapy and physical therapy, among other complementary treatments. The disparity in care between those with and without financial resources is stark, and touch is one of the services these clients invest in. Integrating touch in certain sectors of the mental health field is indeed a complex issue. However, there are many settings where it is both feasible and beneficial, such as private practices, group practices, and some community mental health clinics with relatively high-functioning clients. I believe this enduring taboo around touch is more about habit than necessity, and it's time to reconsider these boundaries. We might need a separate field or license for those working with trauma from a nervous system perspective, or licensing boards could specify when and how such integrations are appropriate. Clinicians working in an integrated manner are generally not operating outside their license but are often fearful due to a lack of clarity. For now, I'll refer to this emerging field as Somatic Trauma and Attachment Therapy (STAT). STATs use:
STATs Treat
Somatic Trauma and Attachment Therapists (STATs) support individuals' personal growth and evolution while recognizing privilege and oppression dynamics and advocating for change in oppressive social systems. STATs receive education, training, and supervision from experienced professionals within the field. This outline represents the current boundaries of STAT practice based on extensive discussions with fellow STATs. I am passionate about continuing to explore and document the evolution of this field, as it is clearly developing its own unique path forward. |
Details
AuthorProsopon Therapy Archives
July 2024
Categories |

 RSS Feed
RSS Feed